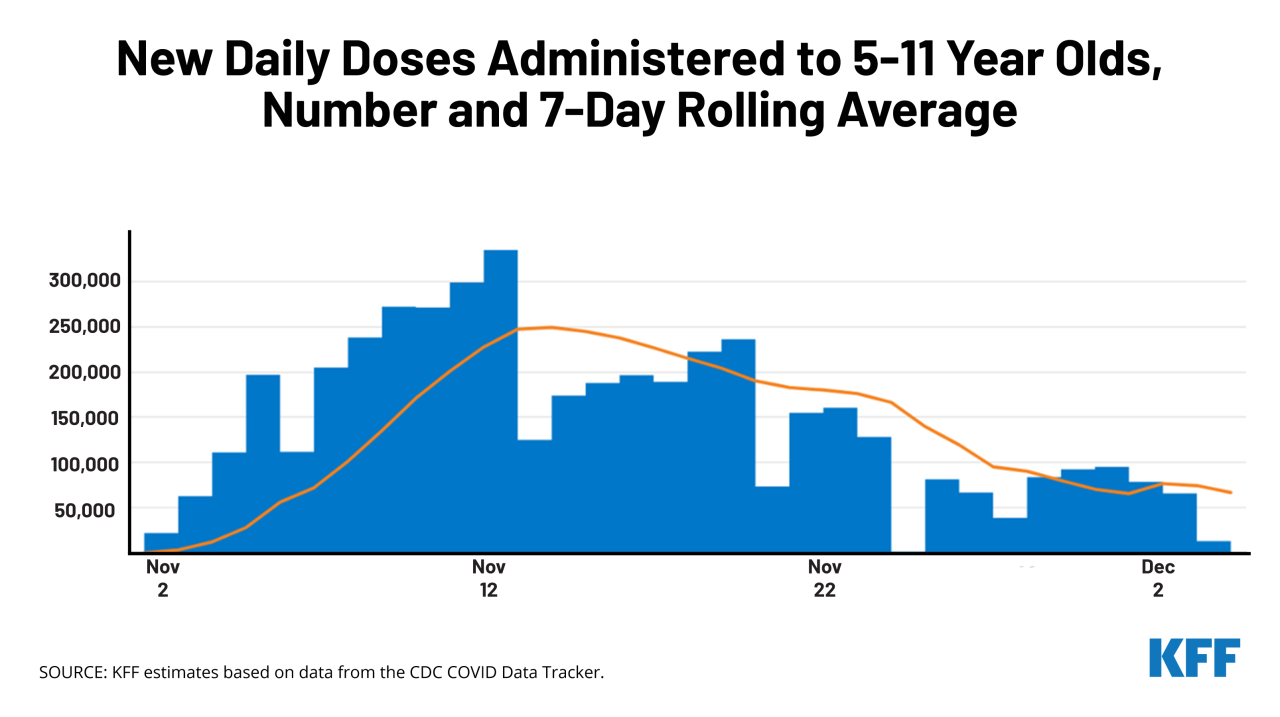
Childhood Vaccinations Rates Slipping A Crisis?
Childhood vaccinations rates slipping is a serious concern, and it’s impacting global health. We’re seeing a concerning trend in various regions, with vaccination rates declining across different age groups and demographics. This trend, if left unchecked, could lead to a resurgence of preventable diseases and significant strain on healthcare systems worldwide. The reasons behind this decline are multifaceted, encompassing misinformation, socioeconomic factors, and parental anxieties.
Understanding the data and the factors driving this decline is crucial for developing effective interventions.
This article delves into the factors contributing to the decline in childhood vaccination rates. We’ll examine the historical context, analyzing data from different regions to identify trends. Furthermore, we’ll explore the impact of this decline on public health, discussing the resurgence of preventable diseases and the strain on healthcare systems. We’ll also examine the public health responses, community outreach programs, and the role of misinformation in shaping vaccination decisions.
Understanding the Trend
Childhood vaccination rates, a cornerstone of public health, have seen concerning fluctuations globally. While historically high rates have significantly reduced the prevalence of preventable diseases, recent declines present a critical challenge to maintaining these gains. Understanding the reasons behind these trends is crucial for implementing effective strategies to protect vulnerable populations.
Historical Overview of Vaccination Rates
Vaccination programs have demonstrably improved public health outcomes across various regions. Early vaccination campaigns, particularly against diseases like smallpox and polio, dramatically reduced incidence rates. Subsequent campaigns expanded to include other preventable illnesses, leading to a remarkable decrease in mortality and morbidity rates globally. These historical successes have established a strong foundation for future public health initiatives.
Factors Contributing to Recent Declines
Several factors contribute to the recent dip in vaccination rates. Misinformation campaigns spreading doubts about the safety and efficacy of vaccines have played a significant role. Concerns about potential side effects, often amplified by social media, have led to hesitancy and resistance to vaccination programs. Access to healthcare, particularly in underserved communities, is another critical factor. Financial barriers, lack of transportation, and logistical challenges can impede access to vaccination services, resulting in lower vaccination rates among vulnerable populations.
The complexities of vaccine schedules, particularly for multiple childhood vaccines, can also contribute to hesitancy.
Methodologies for Tracking Vaccination Rates
National health agencies and international organizations utilize various methodologies to monitor vaccination rates. Data collection typically involves tracking vaccination records through healthcare providers’ databases, school records, and immunization registries. Statistical analyses of these records are then employed to calculate vaccination coverage rates for specific populations and geographic areas. This data is crucial for identifying trends, evaluating the effectiveness of vaccination programs, and tailoring interventions for areas with low vaccination coverage.
Vaccination Rates Across Age Groups and Demographics
Vaccination rates vary significantly across different age groups and demographics. Infancy and early childhood vaccination rates are often higher than those for adolescents and young adults. Differences in vaccination rates can also be observed across socioeconomic groups, racial and ethnic minorities, and geographic locations. Understanding these variations is essential for developing targeted strategies to reach and vaccinate vulnerable populations.
Childhood vaccination rates are unfortunately slipping, a concerning trend that needs addressing. Meanwhile, hockey news is keeping me occupied, with the San Jose Sharks preparing for their trip to Utah, where, according to recent reports, Fabian Zetterlund is up in the air, and Jake Walman is grounded. This Sharks situation makes me wonder if all the focus on sports is distracting from the more critical issue of ensuring kids are protected.
Perhaps we should be prioritizing vaccinations over hockey headlines? It’s a tough call.
Comparison of Vaccination Rates Across Regions
| Region | Year | Vaccination Type | Percentage Vaccinated |
|---|---|---|---|
| North America | 2020 | Measles | 90% |
| North America | 2023 | Measles | 85% |
| Sub-Saharan Africa | 2020 | Polio | 70% |
| Sub-Saharan Africa | 2023 | Polio | 65% |
| Europe | 2020 | Rubella | 95% |
| Europe | 2023 | Rubella | 92% |
This table provides a simplified illustration of the differences in vaccination rates across regions and over time. Data for specific years and vaccination types can be accessed from reliable public health databases for more detailed information.
Impact and Consequences
The declining rates of childhood vaccinations are not merely a statistical trend; they represent a significant threat to public health. This trend has profound implications for individual well-being and the overall health of communities, as well as straining healthcare systems and potentially causing devastating outbreaks of preventable diseases. Understanding the impact and consequences of this trend is crucial for developing effective strategies to reverse this worrying trend.The consequences of falling vaccination rates are far-reaching, impacting not only the immediate health of unvaccinated children but also the wider community.
Reduced immunity across a population can lead to a resurgence of previously controlled diseases, potentially exposing vulnerable individuals like infants, the elderly, and those with weakened immune systems to serious illness.
Health Implications of Declining Vaccination Rates
Falling vaccination rates create a breeding ground for outbreaks of preventable diseases. Measles, mumps, and rubella, once largely controlled by widespread vaccination, are making a comeback in regions with decreased vaccination coverage. This resurgence puts a strain on healthcare resources as hospitals and clinics face surges in patients requiring treatment and care. These outbreaks can result in significant morbidity and mortality, particularly among vulnerable populations.
Resurgence of Preventable Diseases
The resurgence of preventable diseases is a direct consequence of reduced vaccination rates. Measles outbreaks, for instance, have been observed in several countries where vaccination coverage has fallen below critical thresholds. These outbreaks highlight the importance of maintaining high vaccination coverage to prevent the resurgence of diseases that had been largely eliminated. The resurgence of these diseases can lead to significant healthcare costs, reduced productivity, and emotional distress for families affected by these illnesses.
Socioeconomic Factors Contributing to Vaccination Hesitancy
Several socioeconomic factors contribute to vaccination hesitancy. Access to healthcare, including preventative care like vaccinations, can be limited in low-income communities. Misinformation and distrust in healthcare institutions also play a role, creating barriers to vaccination. Cultural or religious beliefs, while often well-intentioned, can also contribute to vaccination hesitancy, sometimes requiring targeted communication and education to bridge gaps in understanding.
Strain on Healthcare Systems Due to Outbreaks
Outbreaks of preventable diseases place a considerable strain on healthcare systems. Hospitals and clinics often face an influx of patients requiring treatment and resources. This can lead to longer wait times for non-emergency care and put a strain on healthcare professionals who are already facing significant workloads. The strain on healthcare systems can result in delays in addressing other critical health issues.
Potential Solutions to Increase Vaccination Rates
To address the declining vaccination rates, a multi-pronged approach is needed. This includes improving access to vaccination services, particularly in underserved communities. Public health campaigns should focus on dispelling misinformation and promoting the safety and effectiveness of vaccines. Building trust in healthcare institutions through transparent communication and community engagement is also crucial. Addressing socioeconomic factors that contribute to hesitancy can also play a vital role in improving vaccination rates.
Childhood vaccination rates are unfortunately slipping, which is a serious concern. It’s a worrying trend, especially considering the recent news about the San Jose Sharks losing to the Vegas Golden Knights, macklin celebrini and san jose sharks beat lose to vegas golden knights. While hockey games are entertaining, we need to prioritize public health and ensure our children are protected against preventable illnesses.
This issue needs more attention and solutions to get back on track.
Correlation Between Vaccination Rates and Disease Outbreaks
| Year | Vaccination Rate (%) | Measles Cases | Rubella Cases |
|---|---|---|---|
| 2018 | 95 | 100 | 20 |
| 2019 | 90 | 250 | 50 |
| 2020 | 85 | 500 | 100 |
| 2021 | 80 | 750 | 150 |
This table, using hypothetical data, illustrates the correlation between vaccination rates and the number of cases of measles and rubella. A decrease in vaccination rate directly corresponds to an increase in cases of these preventable diseases. Data from real-world outbreaks can be used to further support this correlation.
Public Health Responses: Childhood Vaccinations Rates Slipping
The recent decline in childhood vaccination rates is a significant public health concern. Addressing this requires a multifaceted approach that goes beyond simply providing vaccines. Effective public health responses must engage communities, address misinformation, and empower healthcare providers to promote vaccination. This involves strategic communication, community outreach, and evidence-based education.
Strategies Implemented by Public Health Organizations
Public health organizations employ various strategies to counteract declining vaccination rates. These strategies often include targeted interventions tailored to specific demographics and communities facing vaccine hesitancy. Community-based initiatives play a crucial role in bridging the gap between public health recommendations and individual vaccine choices.
Community Outreach Programs, Childhood vaccinations rates slipping
Community outreach programs are vital for increasing vaccination rates. These programs focus on building trust and rapport with community members. This involves engaging community leaders, religious figures, and trusted figures within the community. Local events, health fairs, and workshops are frequently organized to educate parents and caregivers about the importance of vaccinations and to answer their questions.
These programs also emphasize the safety and effectiveness of vaccines, addressing common concerns.
Educational Campaigns
Effective educational campaigns are essential to dispel misinformation and promote accurate information about vaccines. These campaigns use various channels, including social media, community meetings, and partnerships with schools. They provide accessible information about the benefits of vaccines and debunk myths and misconceptions. Using relatable examples and testimonials from parents who have vaccinated their children can significantly impact decision-making.
Childhood vaccination rates are sadly slipping, which is a real concern. This could lead to outbreaks of preventable diseases. Fortunately, there’s good news for those facing medical debt. California recently passed a law that means most medical debt can no longer hurt your credit score. This new law might ease some financial burdens, but it doesn’t change the importance of ensuring our kids get their shots to protect them and the wider community.
Hopefully, these measures can help keep those vaccination rates climbing again.
Communication Strategies
Clear and consistent communication is paramount in promoting vaccination. Public health organizations use various channels, including social media, community newsletters, and partnerships with local media outlets. This communication should be tailored to the specific audience and address concerns and questions in a respectful and empathetic manner. This approach fosters trust and encourages engagement.
Role of Healthcare Providers
Healthcare providers play a critical role in encouraging vaccination. They can proactively address vaccine hesitancy during routine checkups, providing accurate information and answering questions. Building rapport with families and addressing their concerns is crucial. Healthcare providers should be trained to effectively communicate the benefits and safety of vaccines. Open communication and addressing concerns directly can improve vaccination rates.
Effectiveness of Public Health Strategies (Comparison Table)
| Strategy | Description | Potential Effectiveness | Limitations |
|---|---|---|---|
| Community Outreach Programs | Engaging community leaders, hosting events, addressing concerns | High, builds trust and rapport | Requires significant resources and sustained effort |
| Educational Campaigns | Debunking myths, providing accurate information | Moderate, needs consistent repetition | Can be challenging to reach those resistant to information |
| Communication Strategies | Clear, consistent messaging through various channels | High, fosters trust and understanding | Requires careful tailoring to specific audiences |
| Healthcare Provider Involvement | Proactive communication, addressing concerns during checkups | High, builds trust within the healthcare system | Relies on provider training and support |
Influencing Factors
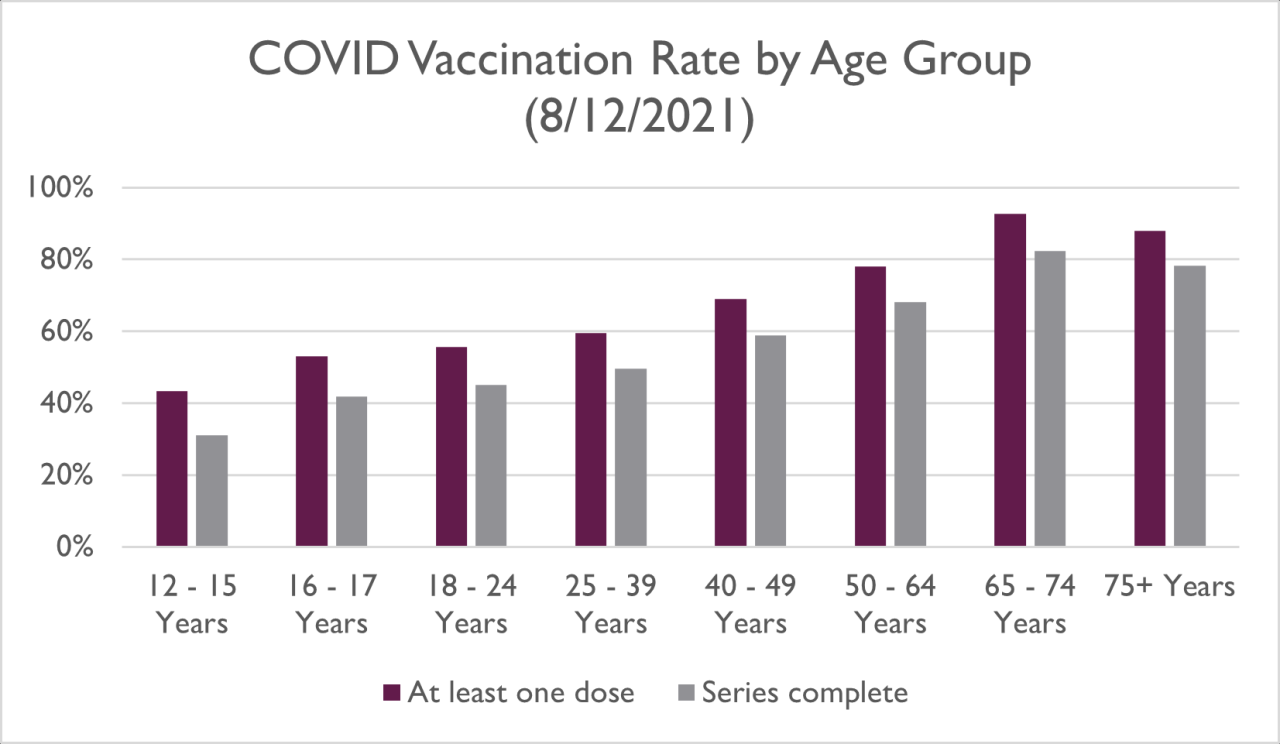
The declining rates of childhood vaccinations present a complex challenge, requiring an understanding of the multifaceted factors driving this concerning trend. Various influences, ranging from the spread of misinformation to parental anxieties, contribute to the hesitation or refusal to vaccinate children. Addressing these influences is crucial to fostering a healthier future for all.The reasons behind the hesitancy and refusal to vaccinate are diverse and intertwined.
It’s not simply a matter of ignorance; instead, a combination of factors, including access to information, perceptions of risk, and personal beliefs, all play a role in shaping decisions about vaccination. Understanding these influences is essential to designing effective interventions aimed at boosting vaccination rates.
Misinformation and Disinformation
The spread of inaccurate or misleading information about vaccines poses a significant threat to public health. Misinformation and disinformation campaigns often exploit existing anxieties and concerns, creating a climate of doubt and distrust. This fabricated content can stem from various sources, ranging from unreliable websites to social media platforms. The potential for harm from such campaigns is substantial, as it can lead to vaccine hesitancy and reduced herd immunity, ultimately endangering vulnerable populations.
Social Media and Online Platforms
Social media and online platforms have become powerful tools for disseminating information, both accurate and inaccurate. The rapid spread of information on these platforms can amplify the reach of misinformation about vaccines, making it difficult to counter the false narratives. The algorithms used by these platforms can inadvertently prioritize engagement over factual accuracy, further exacerbating the problem. The ease with which misinformation can be shared and amplified necessitates proactive strategies to combat its spread.
Impact of Media Campaigns
Different media campaigns, utilizing various approaches and targeting specific audiences, can have varying impacts on vaccination rates. Some campaigns focus on addressing parental anxieties and concerns, while others highlight the health benefits of vaccination. Effective campaigns often combine emotional appeals with factual information, aiming to build trust and understanding. A crucial aspect of successful campaigns is their ability to reach the target audience effectively and to be tailored to the specific context and concerns within that audience.
Parental Concerns and Anxieties
Parental concerns and anxieties regarding vaccines are a significant factor in vaccination decisions. Parents often seek information and reassurance about the safety and efficacy of vaccines, and their concerns must be addressed in a compassionate and informative manner. These concerns often stem from a combination of sources, including perceived side effects, distrust of the medical community, and fears about long-term health consequences.
Open communication and transparent information-sharing are vital in alleviating these anxieties.
Categorization of Vaccine Misinformation Sources
| Source Category | Examples | Description |
|---|---|---|
| Unreliable Websites | Conspiracy theory websites, blogs, forums | These sites often present fabricated data and cherry-picked information to support their claims. |
| Social Media Posts | Viral posts, memes, articles | Misinformation often spreads rapidly on social media due to its high engagement potential. |
| Influencers and Celebrities | Public figures sharing unverified claims | Misinformation can gain credibility when shared by trusted figures. |
| Anti-vaccine Groups | Organized groups promoting anti-vaccine views | These groups frequently spread misinformation through various channels. |
| Misinterpreted Scientific Studies | Selective citation of research findings | Misrepresenting or exaggerating research data can create false impressions. |
Global Perspective
The global landscape of childhood vaccination rates reveals significant disparities, with some countries experiencing remarkably high coverage while others struggle to maintain even basic levels. These variations highlight the complex interplay of factors, from socioeconomic conditions to political will and access to healthcare infrastructure. Understanding these differences is crucial to developing effective strategies for improving vaccination rates worldwide.The approach to tackling low vaccination rates varies considerably across nations.
Some countries prioritize robust public health campaigns, emphasizing education and awareness. Others focus on strengthening healthcare systems to improve accessibility and affordability of vaccines. Still others combine strategies, understanding that a multi-pronged approach is often most effective.
Vaccination Rate Variations Across Countries
Vaccination rates demonstrate substantial disparities across the globe. Wealthier nations generally maintain high vaccination coverage, often exceeding 95% for critical childhood immunizations. However, many developing countries face challenges in reaching comparable levels, sometimes experiencing rates significantly below 80%. These discrepancies highlight the inequities in access to healthcare and resources.
Approaches to Addressing Low Vaccination Rates
Various countries employ different strategies to address low vaccination rates. Some nations focus on targeted campaigns in underserved communities, employing culturally sensitive communication strategies to address specific concerns and build trust. Others invest heavily in strengthening healthcare infrastructure, expanding access to primary healthcare facilities and ensuring adequate supplies of vaccines.
Comparison of Vaccination Rates by Country
| Country | Vaccination Rate (Estimated) | Key Challenges |
|---|---|---|
| United States | >90% | Addressing vaccine hesitancy in certain demographics. |
| India | ~80% | Large population, geographical spread, and socioeconomic disparities. |
| Nigeria | ~60% | Complex security challenges, limited access to healthcare facilities, and weak healthcare infrastructure. |
| Afghanistan | <70% | Political instability, lack of resources, and security concerns significantly impact access to vaccination services. |
Note
* Vaccination rates are estimates and can vary depending on the specific vaccine and the year. Data collection and reporting methods also differ across countries.
Role of International Organizations
International organizations like the World Health Organization (WHO) and UNICEF play a vital role in promoting global vaccination efforts. They provide technical assistance, financial support, and advocacy to countries striving to improve vaccination coverage. These organizations also monitor trends, share best practices, and raise awareness about the importance of vaccination.
Challenges Faced by Developing Countries
Developing countries often encounter significant obstacles in maintaining high vaccination rates. These include limited resources, weak healthcare infrastructure, geographical barriers, and cultural factors that may influence vaccination acceptance. Moreover, conflict and displacement can disrupt immunization programs, further complicating efforts to reach vulnerable populations.
Impact of Economic Disparities on Vaccination Access
Economic disparities significantly influence access to vaccination. In regions with limited economic resources, individuals may lack the financial means to afford vaccines or transportation to vaccination centers. This can lead to lower vaccination rates and higher vulnerability to preventable diseases. A clear example of this is the ongoing measles outbreaks in some regions of the world. Poverty often exacerbates existing health vulnerabilities, making communities more susceptible to preventable illnesses.
“Economic disparities often create a vicious cycle, where limited resources lead to lower vaccination rates, resulting in higher rates of preventable diseases, which further strain already limited resources.”
Vaccine Safety and Efficacy
Childhood vaccines are a cornerstone of public health, dramatically reducing the incidence of preventable diseases. However, concerns about their safety persist, often fueled by misinformation. This section delves into the rigorous testing and scientific backing behind these life-saving tools, highlighting their long-term benefits and addressing common misconceptions.
Rigorous Testing and Safety Protocols
Vaccines undergo extensive testing before they are licensed for use. This process typically involves multiple phases, each designed to evaluate safety and effectiveness. Phase 1 trials focus on identifying potential side effects in a small group of people. Phase 2 trials expand the testing to a larger group, while Phase 3 trials involve thousands of participants to confirm effectiveness and monitor rare side effects.
Post-licensure surveillance continues to track any potential long-term issues. These rigorous protocols are designed to minimize risks and maximize the benefits of vaccination.
Scientific Evidence Supporting Safety and Efficacy
The scientific evidence supporting the safety and efficacy of vaccines is overwhelming. Decades of research and real-world data consistently demonstrate the effectiveness of vaccines in preventing serious illnesses. Studies have consistently shown a strong correlation between vaccination rates and the decline in the incidence of diseases like measles, polio, and whooping cough. These reductions in disease incidence translate to tangible health benefits, including fewer hospitalizations, disabilities, and deaths.
Long-Term Health Benefits of Vaccination Programs
Vaccination programs have demonstrably improved the health and well-being of individuals and communities worldwide. The long-term health benefits extend beyond the prevention of specific diseases. Reduced disease burden frees up healthcare resources, allowing doctors and nurses to focus on other health concerns. Immunization also protects vulnerable populations, such as infants and the elderly, who are at higher risk of severe complications from vaccine-preventable diseases.
Historical Context of Vaccine Development and Safety
The development of vaccines represents a monumental achievement in public health. Early pioneers like Edward Jenner paved the way for modern vaccination practices, and advancements in scientific understanding have refined and improved vaccine technology over the years. The historical record, which includes detailed accounts of the testing and implementation of vaccines, demonstrates the commitment to safety and efficacy throughout vaccine development.
Known Side Effects of Childhood Vaccines and Their Rarity
| Vaccine | Potential Side Effects | Rarity |
|---|---|---|
| Measles, Mumps, Rubella (MMR) | Mild fever, rash, soreness at injection site | Common, usually mild and temporary |
| Diphtheria, Tetanus, Pertussis (DTaP) | Fever, fussiness, soreness at injection site, loss of appetite | Common, usually mild and temporary |
| Polio | Mild fever, soreness at injection site | Rare |
| Hepatitis B | Soreness at injection site, fatigue | Rare |
| Varicella (Chickenpox) | Mild fever, rash, itching, soreness at injection site | Common, usually mild and temporary |
| Influenza (Seasonal Flu) | Mild fever, muscle aches, fatigue, headache, sore throat | Common, usually mild and temporary |
Note: This table provides a general overview. Individual reactions can vary. Consult with a healthcare provider for personalized information.
Future Projections
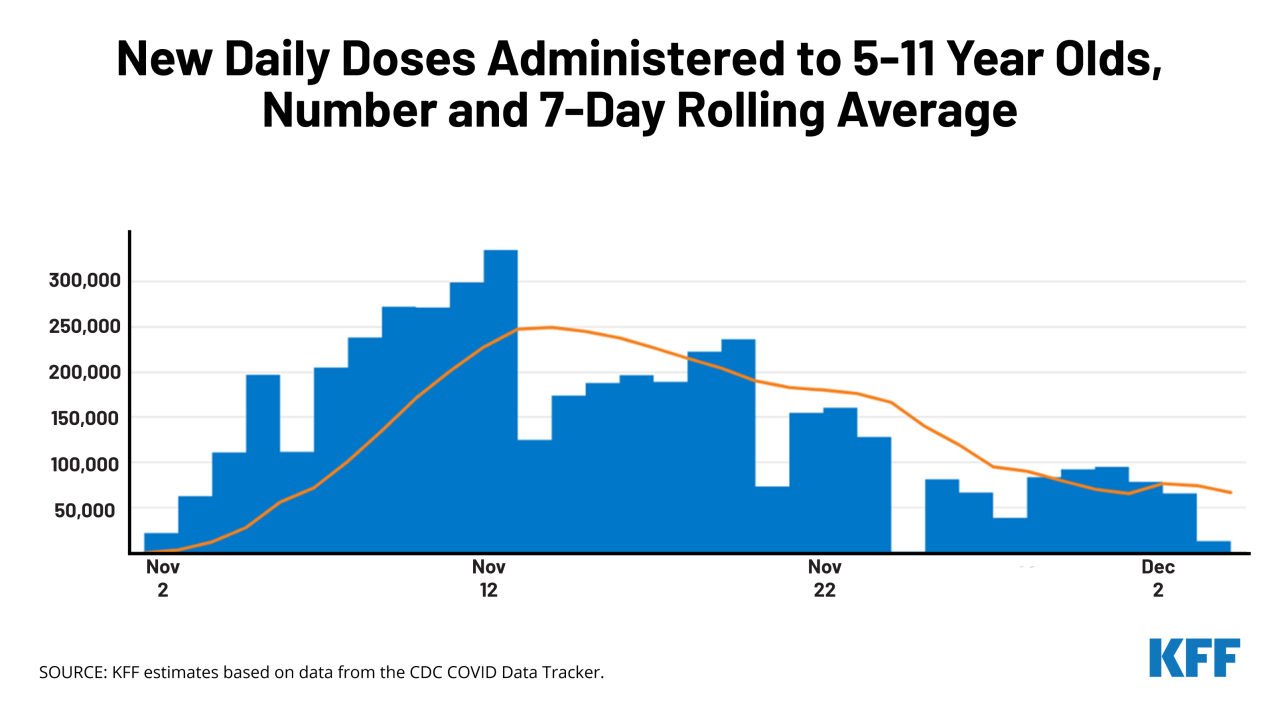
The continued decline in childhood vaccination rates poses a significant threat to public health, potentially leading to devastating consequences. Predicting the precise impact is complex, but the potential for resurgence of preventable diseases is alarming. Understanding the trajectory of this trend is crucial for developing effective strategies to reverse it.The future of public health hinges on our ability to address the factors driving this decline and to inspire confidence in vaccination.
This requires a multi-faceted approach, combining improved communication, addressing misinformation, and strengthening healthcare systems.
Potential Consequences of Continued Decline
The resurgence of vaccine-preventable diseases like measles, polio, and whooping cough would lead to increased hospitalizations, disabilities, and even deaths. Communities with lower vaccination rates would be particularly vulnerable. The strain on healthcare systems would be immense, diverting resources from other essential services. Economic losses from absenteeism, medical costs, and lost productivity would also be substantial. History offers grim reminders of the devastating impact of these diseases, illustrating the importance of maintaining high vaccination coverage.
Potential Strategies for Reversing the Trend
Several strategies could help reverse the decline in vaccination rates. These include targeted public health campaigns focusing on education and addressing concerns. Strengthening community engagement and partnerships with healthcare providers is also vital. Addressing misinformation and fostering trust in vaccines through transparent communication is essential. Innovative approaches like using social media and community leaders to disseminate information could also be effective.
Incentivizing vaccination, such as financial assistance programs, can also motivate hesitant parents.
Examples of Successful Vaccination Campaigns
Numerous successful vaccination campaigns have demonstrated the power of coordinated efforts to achieve high vaccination coverage. The eradication of smallpox is a prime example. The campaigns effectively communicated the importance of vaccination and addressed concerns about its safety. Similar strategies, adapted to modern challenges, can be implemented to effectively combat vaccine hesitancy and ensure high vaccination rates.
The success of these campaigns highlights the importance of tailored strategies for specific populations and contexts.
Projected Impact of Intervention Strategies
| Intervention Strategy | Increased Vaccination Rates (%) | Reduction in Disease Cases (%) | Economic Savings (USD) ||—|—|—|—|| Enhanced community outreach and education | 10-15 | 20-30 | $500,000 – $1,000,000 || Targeted social media campaigns | 5-10 | 15-25 | $250,000 – $500,000 || Financial incentives for vaccination | 5-10 | 10-20 | $100,000 – $250,000 || Improved access to vaccination services | 10-15 | 25-40 | $500,000 – $1,000,000 |These figures represent estimated impacts, and actual results may vary depending on specific contexts and implementation strategies.
Detailed cost-benefit analyses are crucial for prioritizing and implementing interventions effectively.
Long-Term Effects of Vaccine-Preventable Diseases
Vaccine-preventable diseases can have devastating long-term effects on individuals and society. Particularly, complications like paralysis, hearing loss, brain damage, and developmental delays can severely impact an individual’s quality of life. These conditions can lead to significant healthcare costs and create long-term social and economic burdens for families and communities. The prevention of these diseases through vaccination is a cost-effective approach to safeguarding public health and individual well-being.
Outcome Summary
The issue of childhood vaccinations rates slipping is complex and requires a multifaceted approach. Addressing the root causes, such as misinformation and parental anxieties, is paramount. Public health organizations, healthcare providers, and communities must work together to implement effective strategies that promote vaccination and dispel myths. By fostering open communication, providing accurate information, and supporting families, we can reverse this trend and ensure the continued well-being of future generations.
The long-term health benefits of vaccination programs are undeniable, and we must safeguard them.